Vaginal Steaming in Pelvic Organ Descent
As a physiotherapist dedicated to urogynaecological, obstetric and reproductive topics, I highly recommend the vaginal steaming and I have had very good experience and results with it. However, there are situations and conditions where you need to use the steaming with caution and consult individually your health condition with other specialists. Such as with a diagnosis of pelvic organ descent.
What's it about?
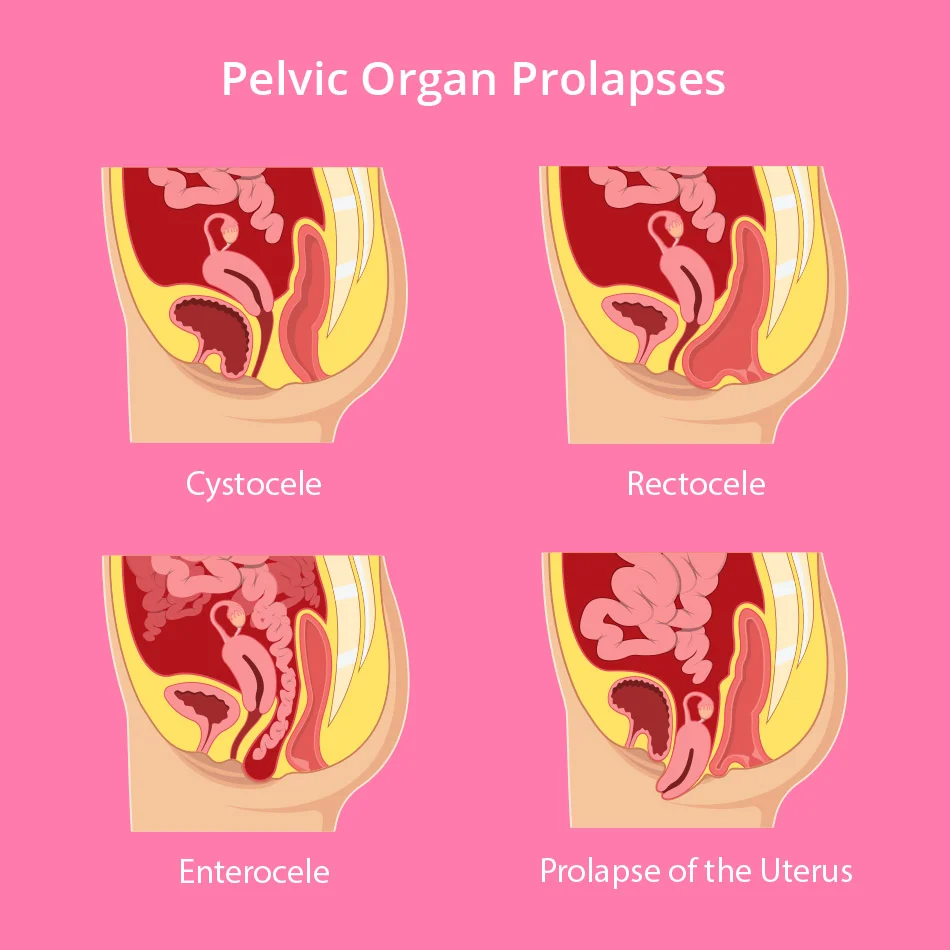
Pelvic organ descent or pelvic organ prolapse is any change in the position of an organ lying in the pelvis. This is the bladder with the urethra, the uterus with the vagina and the end of the colon with the rectum. Different degrees of descent are then distinguished according to the size of the descent, from lighter to severe forms.
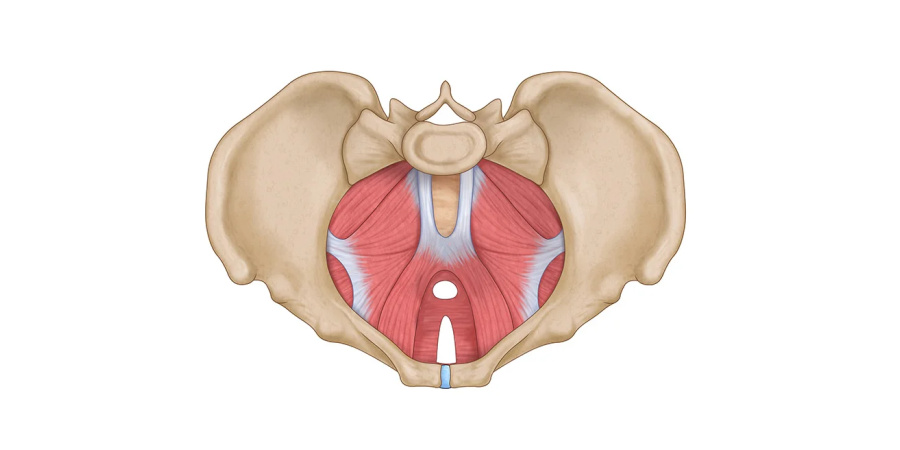
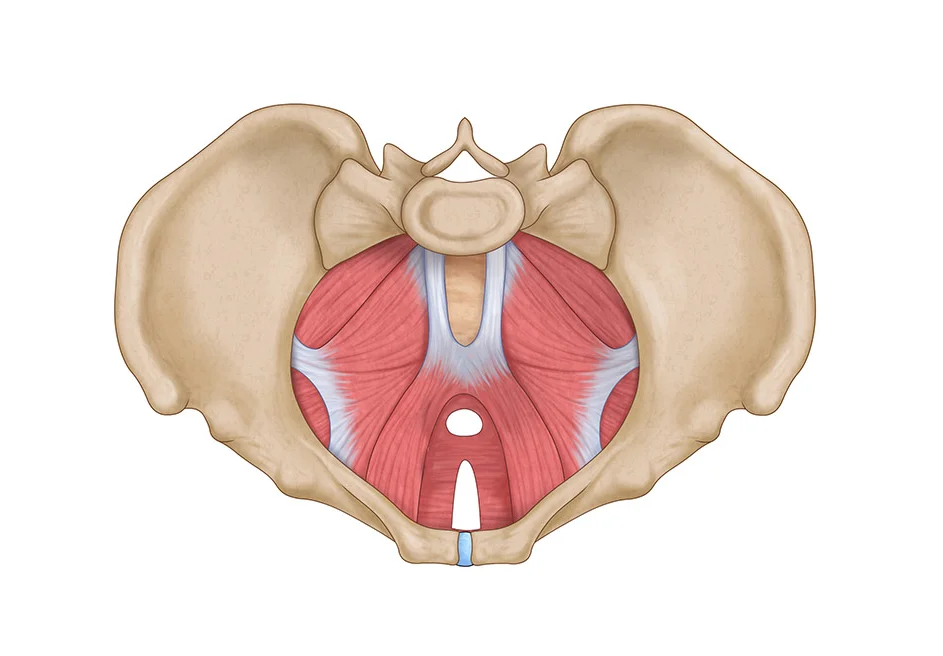
The pelvic floor can be thought of as a trampoline. The bones form the rigid structure of the trampoline, the springs are the ligaments and tendons and the "mat" itself is the soft pelvic floor (muscles, nerves, blood vessels). The pelvic organs lie on just such a trampoline. If we put unreasonable pressure on the trampoline (usually repeatedly) and do not perform regular servicing, one day the trampoline will fail - the mat will fall down, it will not be springy, the spring will break off, the structure will collapse...
Causes of occurrence
The cause of the descent is either a malfunction of the pelvic floor (the mat is too tight or too loose) or a malfunction of the pelvic floor structure (broken spring, broken bar structure...)
Structural disorders imply more challenging problems when pelvic floor structures are injured. Pelvic floor includes not only the muscle mass, but also ligaments, tendons, insertions, suspension apparstus of organs, pelvic bones, nerves, blood vessels and the lymphatic system. All of these affect the functioning of (not only) the reproductive and excretory systems. Structural disorders are caused by various injuries, surgical interventions, difficult birth (often instrumental - vacuum extraction), forceps, pressure on the abdomen, inappropriate birth position...).
As a consequence of descent, incontinence, inflammatory conditions, pain, feeling of pressure or "extra something" in the pelvic or genital area, sexual difficulties, menstrual difficulties, fertility problems, difficulties during pregnancy and also during and after childbirth often occur.
I could write a whole book on the emotional consequences and the impact on quality of life.
What can we do about it?
Firstly, we need to muster the courage not to tackle this situation on our own. I am fully aware that it is psychologically challenging for many women to deal with such an intimate matter with other people. But it is important and necessary because these conditions tend to get worse if not addressed in time.
A medical examination (urogynaecologist or proctologist - dealing with the rectal area) is important. The doctor will assess whether the injury is functional or structural and choose surgical or conservative treatment accordingly.
Physiotherapy is an integral part of both surgical and conservative treatment. However, just as it is with other physicians, it is necessary for the physiotherapist to specialise in this area. Quality physiotherapy does not only deal with the pelvic floor area, but the whole body setup, you need to be taught how to use your body in your life (= individually). That is to say, to move optimally and to be able to adjust your body in different activities and positions so that the problems gradually diminish or disappear altogether. An empathetic and caring approach should be an integral part of this very intimate issue. Therefore, look not only for experts but also for a humane approach in taking care of yourself.
How and when to use the vaginal steaming for descent
I do not recommend vaginal steaming in connection with the descent in the following cases:
-
for moderate and severe descent
-
for untreated descent (without examination, main treatment and recommendations from caring professionals)
-
for significantly flaccid pelvic floor muscles
However, even for these conditions, the situation must be assessed individually, therefore it is possible that if a woman is in care and already knows how to take care of herself adequately, the steaming may be recommended (under certain conditions)
For mild descents and some more difficult cases I can recommend the steaming, but you need to set some limits and adjust the conditions under which the steaming is done:
-
If you are not under the care of a gynecological physiotherapist and a doctor, it is necessary to visit them before the application of the vaginal steaming, to find out the situation and choose the appropriate main treatment. It is possible that the steaming will be recommended only after pelvic floor tension and function have been corrected, i.e. after exercise and education of movement behaviour and lifestyle changes
-
If the steaming is recommended, the appropriate position, length of the steaming and temperature of the decoction should be chosen, or specific herbs should be selected appropriately
-
The general contraindications of the steaming still apply
-
It is necessary to be instructed on how to carry out the vaginal steaming
-
If the vaginal steaming is not working well for you, stop doing it and consult the situation with your caring professionals and a trained steaming provider

Position, temperature, length of the steaming
Sitting position on the steaming chair
If organ descent is diagnosed, it is necessary to trace when the descent worsens. It is a good idea to try a position where the pelvis is parallel to the ground and the spine is straight - the knees are approximately at the same level as the pelvis. For some types of descent, it helps to put an even smaller box under your feet so that your knees are higher than your pelvis. However, I don't recommend staying in this position for long and you need to monitor whether the descent is getting worse. Conversely, for other women, it may help if the pelvis is higher than the knees and the trunk is in a slight forward bend. If you are unsure if the descent is getting worse, it is possible to ask the physiotherapist to examine you in these positions and choose the optimal position for you. I always recommend actively supporting the feet in sitting positions, which creates stable support for the pelvis, and then the descent usually does not worsen in these positions. Physiotherapists will teach you how to activate and support the feet.
As for the length of the steaming, until you know how the steaming affects you, make it short - 10 minutes maximum, shorter in the sitting position if you perceive that the descent is getting worse.
Then observe how your condition has changed.

In weakened and hypotonic (reduced tension) pelvic floor, the situation may become worse as the soft tissues become even more loose with the strain. Then you still need to practice and work on your condition with a physiotherapist for some time, and it is possible that the steaming may not be suitable for you in the future (but with the right therapy and under certain steaming conditions I don't think so). On the other hand, for a descent that is accompanied by increased tissue tension, the steaming can nicely relax and improve pelvic sensation.
If you are pregnant and suffer from pain, are incontinent (i.e. even a drop of urine cannot be controlled when you sneeze or cough), or have already been diagnosed with a descent or pelvic floor disorder, I recommend consulting and being taken care of gynaecological physiotherapist before the vaginal steaming. The minimum period of physiotherapy to see results is usually within 3 months, so don't leave your decision to do something about your problems for until a week before your due date.
Summary

Mgr. Pavla Filipová, DiS.
physiotherapist
https://fyziofemina.webnode.cz/





